Scorpion venom could help Bellevue doctors fight cancer
Published 2:25 pm Friday, March 11, 2016
A new clinical trial at Overlake Medical Center is testing whether scorpions hold the key to more effectively targeting cancer cells during surgeries.
“We live in such an exciting time that people are continually looking at drugs to respond to tumor threats,” said Overlake Medical Center surgeon, Dr. Kristi Harrington. “That’s the good thing about being diagnosed with a cancer in this day and age. It’s so hopeful compared to what it used to be.”
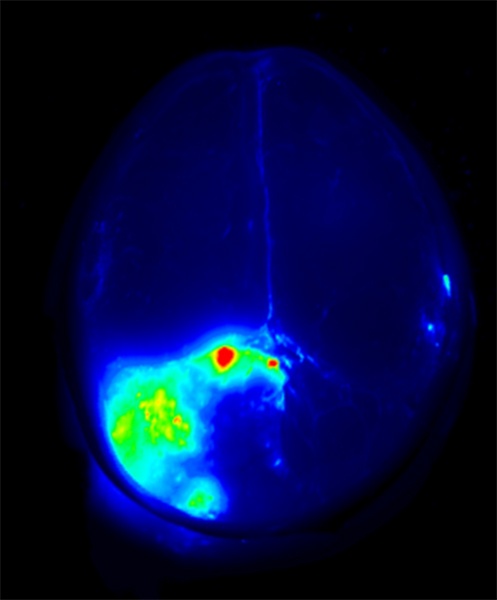
Harrington is one of a handful of surgeons across the country participating in a phase one trial of a “tumor paint” — a florescent dye that is attached to a peptide found in scorpion venom that mysteriously binds to cancerous cells, in theory lighting them up on scans and allowing surgeons to be better able to remove the cells during surgery.
Surgeons at Overlake, Seattle Children’s Hospital, Cedars-Sinai Medical Center in Los Angeles, California and the NEWRO Foundation in Brisbane, Queensland, Australia are participating in the clinical trial.
In addition to testing it on breast cancer cells, Overlake surgeons have also tested the paint on lung, kidney, prostate and rectal cancer cells. The tumor paint is also being tested on pediatric brain tumors at Seattle Children’s.
Currently, the scorpion peptide is injected into the bloodstream during surgery so that the tissue removed during surgery can be examined to see how well the paint bound to cancer cells.
The peptide could mean that cancer surgeons may one day be able to tell patients’ loved ones that they are certain they got everything.
Currently, surgeons rely on scans to make educated guesses where the cancer cells are located, as they are invisible to the naked eye.
“I can’t see the tumor, and in a lot of cases, because breast cancer patients are often diagnosed so early through a mamogram or ultrasound or MRI, I can’t feel it either,” Harrington said. “Any cells that are missed could have negative consequences, which is why patients who only have lumpectomies removing the tumor instead of the entire breast often have radiation after surgery.
“Maybe someday, if tumor paint or something like it proves to be efficacious, you’ll be pretty comfortable that you didn’t leave everything, so then you won’t have to do radiation. I don’t know — I wish I had a crystal ball,” she said.
Researchers aren’t precisely certain why the peptide potentially binds better to cancer cells than normal cells, as preliminary results indicate. Their current theory is that the peptide binds to certain proteins that are normally inside of cells, but moves to the exterior membrane of cancer cells, according to Dennis Miller, the senior vice president of development at Blaze Bioscience, which is conducting the clinical trial.
There was a big push for researchers to look for natural products with medical purposes in the 80s and 90s, Miller said, but it sometimes takes a while to understand the full range of uses for these products.
A group of researchers at the University of Alabama began probing the uses for this scorpion peptide in the early 90s before Jim Olson, a brain cancer researcher at Fred Hutchinson, began wondering if it would be possible to highlight cancer cells.
After years of development, the tumor paint was approved by the Food and Drug Administration in September 2014.
“Any patient who is diagnosed with cancer, that’s a very scary thing to have a physician tell you that,” Miller said. “We’re trying to give the cancer surgeons a new tool to help the patients who are fighting cancer. We want to give them the best start at the very beginning of their cancer care to get the best possible outcome.”
The tumor paint is currently in the initial stages of their clinical trial. Blaze Bioscience expects to complete their phase one testing by the end of this year, and complete their clinical trial by mid-2018.